Medication errors happen more often than many people might imagine. A recent study from the BMJ estimates that more than 237 million medication errors are made every year in England.
Researchers labelled these “definitely avoidable” and calculated a cost of nearly £98.5 million to the NHS every year. Even more concerning is that these errors are estimated to have led to the loss of 1,708 lives.
What are the main causes of medication errors?
The Care Quality Commission (CQC) — the independent regulator of all health and social care services in England – identified six areas of medicine risk, which include:
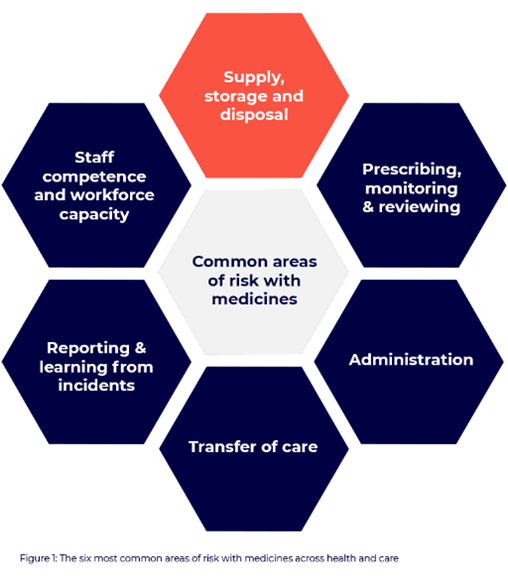
Protecting against error requires a systematic approach. In a recent interview with the Pharmaceutical Journal, Sarah Billington, head of medicines optimisation at the CQC spoke about what it takes to pass a CQC inspection. She explained how the fundamental standards are assessed by asking five questions: ‘Is it safe? Is it effective? Is it caring? Is it well led? And is it responsive?’
In busy and demanding environments, especially over the period of the pandemic, medicine checks and follow-ups can be missed. Handovers between shifts can interrupt processes and new or temporary staff may not be familiar with procedures.
In these conditions., it’s perhaps not surprising to see examples of teams falling short of best practice. The problem is that medication errors can have serious consequences. In one critical report into an NHS facility, the CQC stated: “We found that a wide range of medicines were not always stored appropriately, including intravenous fluids and controlled drugs. We also found that some medicines were not stored at the manufacturer’s recommended temperature, which can compromise their effectiveness and pose a risk to patient safety.”
Supporting frontline NHS teams
Frontline staff need support in this area and technology is proving to be a powerful ally in medicine optimisation. The latest innovations not only automate temperature monitoring of fridges and freezers but provide staff with a process to follow in the event of a critical temperature variation. This helps to ensure the right remedial action is taken – and creates a digital audit trail.
On the subject of medicine storage, the CQC says “inspectors may also ask to see evidence of the log of fridge temperatures, maintenance checks and a policy for what to do if a temperature breach occurs”.
Using digital workflow tools in place of traditional paper checklists means that frontline staff receive alerts of temperature excursions in real-time and instructions on what to do next, ensuring the right thing is done by the right person at the right time and place.
Responding to incidents
By providing staff with corrective-action workflows and policies, NHS providers are ensuring best practice and empowering NHS staff to deliver the best possible patient care. They also generate real-time audit trails, to make auditing easier replacing traditional methods of data collection that can be time intensive and susceptible to human error.
At Checkit, our mission is to support NHS teams with digital monitoring and process tools, so they feel empowered to keep patients safe and keep avoidable costs to a minimum.
Our monitoring technology is being used by 43% of NHS Trusts. One of these is Birmingham & Solihull NHS Foundation Trust. The Trust’s Director of Pharmacy and Medicines Management, Nigel Barnes, said: “With the previous thermometers we didn’t know how long any temperature excursion may have lasted for. Now I know exactly what the breach was, where it was and how long it lasted, so I can make better judgments about the next steps. If a ward contacts us, we can see the graphs and advise accordingly.”
We’ve seen how monitoring and workflow tools support the core duties of frontline staff, and provide managers with new levels of insight, giving them the ability to be effective and responsive in their policies and procedures.


